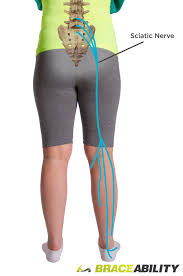
Sciatica is a shooting pain from back, radiates into the buttock and down the back of one leg. The pain is often caused by pressure on the sciatic nerve from a herniated disc, bone spurs or muscle strain (Fig. 1). You play an important role in the prevention, treatment, and recovery of leg pain. It typically improves with rest, physical therapy, and other self-care measures. Chronic pain may be helped with surgery.

Figure 1. The sciatic nerve is formed from the spinal nerves L4 to S3. The two sciatic nerves travel through the pelvis and down the back of each leg. Each nerve divides into a peroneal and tibial nerve to provide feeling and muscle control of the legs and feet.
Types of leg pain
Leg pain ranges from mild to severe and can be acute or chronic.
Acute sciatic pain occurs suddenly and usually heals within several days to weeks. The severity relates directly to the amount of tissue injury. The source of pain may be in the spinal joints, discs, nerves, or muscles and ligaments.
Chronic sciatic pain persists for more than 3 months and its source may be hard to determine. Chronic pain may be felt all the time or worsen with certain activities. Contributing factors may include nerve damage, tissue scarring, arthritis, or mental effects of pain. People with chronic symptoms may be referred to a pain specialist
What are the symptoms?
Classic sciatic pain starts in the low back and buttocks. It affects one leg traveling down the back of the thigh, past the knee, and sometimes into the calf and foot. The pain feels worse in the leg than in the back. It may range from a mild ache to severe burning or a shooting pain. Numbness or tingling (pins-and-needles) can occur in your leg and foot. This usually is not a concern unless you have weakness in your leg muscles or foot drop.
Sitting usually causes the most pain because of the weight this position puts onto the discs. Activities, such as bending or twisting, worsen the pain, whereas lying down tends to bring relief. Running or walking may actually feel better than sitting or standing for too long.
Seek medical help immediately if you have extreme leg weakness, numbness in the genital area, or loss of bladder or bowel function. These are signs of a condition called cauda equina syndrome.
What are the causes?
Sciatica can be caused by a number of conditions that irritate or compress the sciatic nerve:
- Piriformis syndrome: Tightening or spasm of the piriformis muscle can compress the nerve.
- Trauma: A sports injury or fall can fracture the spine or tear a muscle and damage nerves.
- Herniated disc: The gel-like center of a spinal disc can bulge or rupture through a weak area in the disc wall and compress nerves.
- Stenosis: Narrowing of the bony canals in the spine can compress the spinal cord and nerves.
- Osteoarthritis: As discs naturally age they dry out and shrink. Small tears in the disc wall can be painful. Bone spurs can form. The facet joints enlarge and ligaments thicken.
- Spondylolisthesis: A weakness or stress fracture in the facet joints can allow a vertebra to slip out of position and pinch the nerves.
Leg pain can also be caused by a joint problem in the hip or sacroiliac joint. This type of referred pain is quite common, but is not sciatica.
How is a diagnosis made?
A careful medical exam will attempt to determine the type and cause of your spine problem and the treatment options. A diagnostic evaluation includes a medical history and physical exam. Sometimes imaging scans (e.g., x-ray, CT, MRI) and tests to check muscle strength and reflexes are used.
What treatments are available?
Healing begins with self-care and nonsurgical strategies (Fig. 2). The goal is to correct the problem, restore function, and prevent re-injury.

Figure 2. Exercise, strengthening, stretching and ideal weight loss are key elements to your treatment. Make these a part of your life-long daily routine.
Self care: Sciatica often resolves with rest, ice or heat, massage, pain relievers, and gentle stretches. Reduce muscle inflammation and pain using an ice pack for 20 minutes several times a day during the first 48 to 72 hours. Thereafter, a warm shower or heating pad on low setting may be added to relax the muscles. A short period of bed rest is okay, but more than a couple of days does more harm than good. If self-care treatments aren’t working within the first couple of days, see your doctor.
Medication: Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin, ibuprofen or naproxen, can bring relief. A muscle relaxant may be prescribed for spasms. If pain is severe, an analgesic may be prescribed that can be taken with the NSAID or muscle relaxant.
Steroids can reduce the swelling and inflammation of the nerves. They are taken orally (as a Medrol dose pack) tapered over a five-day period or by injection directly into the painful area (see epidural steroid injections and facet injections). Steroids may provide immediate pain relief within 24 hours.
Physical therapy: For most leg pain, we recommend a nearly normal schedule from the onset. Physical therapy can help you return to full activity as soon as possible and prevent re-injury. Physical therapists will show proper lifting and walking techniques, and exercises to strengthen and stretch your lower back, leg, and stomach muscles. Massage, ultrasound, diathermy, heat, and traction may also be recommended for short periods. Patients may also benefit from yoga, chiropractic manipulation and acupuncture.
Surgery: Surgery is rarely needed unless you have muscle weakness, a proven disc herniation, cauda equina syndrome, or severe pain that has not resolved after a reasonable course of nonsurgical treatment. Surgery for a herniated disc, called a discectomy, removes the portion of the disc compressing the spinal nerve. People with stenosis may benefit from a decompression of the nerves.
Recovery and prevention
A positive mental attitude, regular activity, and a prompt return to work are all very important elements of recovery. If regular job duties cannot be performed initially, modified (light or restricted) duty may be prescribed for a limited time.
Prevention is key to avoiding recurrence:
- Proper lifting; avoid sitting for long periods
- Good posture during sitting, standing, moving, and sleeping
- Regular exercise with stretching and strengthening
- An ergonomic work area
- Good nutrition, healthy weight and lean body mass
- Stress management and relaxation
- No smoking